
Breast cancer, a complex and deeply personal journey, impacts countless lives each year. In the midst of this challenge, finding the right care and expertise is paramount. This is where Texas Breast Center, under the leadership of Dr. Valerie J. Gorman, emerges as a beacon of hope and excellence. Dr. Gorman, a renowned breast surgeon certified by the American Board of Surgery, embodies a unique blend of skill, compassion, and dedication. As Chief of Surgery and Medical Director of Surgical Services at Baylor Scott & White Medical Center – Waxahachie, her approach is not just about treating a disease but about caring for the person behind it.
The ethos of Texas Breast Center is grounded in offering an advanced, personalized, and targeted approach to breast surgery and cancer treatment. For you, the patient, this means receiving care that’s tailored to your specific needs and circumstances, ensuring the most effective treatment journey. Dr. Gorman’s expertise in surgical oncology, coupled with her commitment to patient-centric care, ensures that each patient’s experience is rooted in empathy, understanding, and the highest standard of medical excellence. This introduction to Texas Breast Center and Dr. Gorman’s work aims to guide and inform you, offering insights into how their approach can significantly benefit your journey through breast cancer treatment.
Questions to Ask a Dallas Breast Cancer Surgeon
When seeking the best breast cancer surgeon in Dallas, it’s important to ask the right questions to ensure you receive the highest quality of care. Here are some key questions to consider, answered by Dr. Valerie J. Gorman and the Texas Breast Center:
What are your qualifications and experience in breast cancer surgery?
Generally, a qualified breast cancer surgeon should be board-certified and have extensive experience in surgical oncology, specifically in breast surgeries. Dr. Gorman is board-certified by the American Board of Surgery and has a focused specialization in surgical oncology and surgical diseases of the breast. Her experience as Chief of Surgery and Medical Director of Surgical Services at Baylor Scott & White Medical Center – Waxahachie further validates her expertise.
How do you approach treatment planning for breast cancer patients?
A top surgeon should emphasize a personalized treatment plan, considering the patient’s medical history, type of breast cancer, and individual needs. At Texas Breast Center, Dr. Gorman prioritizes a tailored approach. She evaluates each patient’s unique situation to develop a targeted treatment plan, ensuring it aligns with both medical and personal needs.
What types of breast cancer surgeries do you perform?
It’s crucial that your surgeon is skilled in various breast cancer surgeries. Dr. Gorman is proficient in a wide range of procedures, from lumpectomies to mastectomies, ensuring that each surgery is suited to the specific type of breast cancer and patient preference.
Can you describe your post-operative care and follow-up process?
Post-operative care is as important as the surgery itself. At Texas Breast Center, Dr. Gorman and her team provide comprehensive post-operative care, including regular follow-ups, to monitor recovery and address any concerns promptly.
How do you incorporate new technologies or treatments into your practice?
Staying abreast of the latest medical advancements is vital. Dr. Gorman integrates the latest technologies and treatment modalities into her practice at Texas Breast Center, ensuring her patients receive the most advanced care available.
What support services are available for patients?
Holistic care often includes support services like counseling or therapy. Texas Breast Center, under Dr. Gorman’s guidance, offers various support services, acknowledging the emotional and psychological aspects of dealing with breast cancer.
By asking these questions, you can gain a comprehensive understanding of a surgeon’s expertise and approach to care, helping you make an informed decision. Dr. Gorman’s responses highlight the commitment of Texas Breast Center to provide exceptional, personalized care for each patient.
Why did Texas Breast Center choose to be close to Dallas?
Texas Breast Center’s decision to be situated near Dallas is a strategic one, influenced by a combination of factors that align with their mission to provide exceptional breast cancer care.
- Access to a Larger Population: Dallas is one of the largest cities in Texas, offering a vast and diverse population base. Being close to such a metropolitan area allows Texas Breast Center to serve a larger community, extending its reach to more patients who can benefit from their specialized breast cancer care.
- Healthcare Infrastructure: Dallas is known for its robust healthcare infrastructure, including advanced medical facilities, research institutions, and a network of healthcare professionals. This environment fosters collaboration, innovation, and access to the latest medical advancements, which are crucial for a specialty center like Texas Breast Center.
- Patient Convenience: For patients undergoing treatment, proximity to a major city like Dallas means easier access to comprehensive care. It reduces travel time and stress, especially important for those requiring frequent visits or long-term treatment plans.
- Professional Opportunities: Being near a major urban center like Dallas attracts top medical professionals and allows for continuous professional development. This ensures that Texas Breast Center can maintain a team of highly skilled and up-to-date professionals, like Dr. Gorman, who are well-versed in the latest techniques and treatments in breast cancer care.
- Community Engagement and Awareness: Being close to Dallas also allows Texas Breast Center to engage more effectively with the community in terms of education and awareness programs about breast cancer. This is essential for early detection and prevention strategies, which are key components of effective breast cancer management.
Overall, Texas Breast Center’s location near Dallas is a thoughtful choice that reflects our commitment to providing accessible, advanced, and patient-centric breast cancer care, leveraging the advantages offered by a major metropolitan area.
Dallas Breast Cancer Surgery
Breast cancer surgery is a critical component of breast cancer treatment, and its approach can vary significantly depending on the individual case. At Texas Breast Center, led by Dr. Valerie J. Gorman, the approach to breast cancer surgery is centered around the patient’s unique needs and the specifics of their diagnosis.
Dr. Gorman, a board-certified breast surgeon, specializes in a range of surgical procedures that target breast cancer. Her expertise encompasses both lumpectomies, which involve the removal of the tumor and some surrounding tissue, and mastectomies, where the entire breast is removed. The choice between these procedures depends on various factors such as the size and location of the tumor, the stage of the cancer, and the patient’s personal preferences and overall health.
What sets Dr. Gorman and Texas Breast Center apart is their commitment to a personalized approach. Each patient’s surgery plan is carefully crafted, taking into consideration not only the medical aspects of their cancer but also their emotional and psychological well-being. Dr. Gorman believes in empowering her patients with information and involving them in the decision-making process, ensuring that they are comfortable and confident in their treatment plan.
Furthermore, the use of advanced surgical techniques and technology is a hallmark of Dr. Gorman’s practice. She stays abreast of the latest developments in surgical oncology to provide her patients with the most effective, minimally invasive options available. This not only improves the surgical outcomes but also aids in quicker recovery and better cosmetic results.
Post-surgery, the care at Texas Breast Center continues with a thorough follow-up regimen. Dr. Gorman and her team closely monitor the patient’s recovery, addressing any complications and providing support throughout the healing process. The goal is to ensure that each patient not only survives but thrives after breast cancer surgery, with the best possible quality of life.
In summary, breast cancer surgery at Texas Breast Center under Dr. Gorman’s guidance is more than a medical procedure. It is a comprehensive, compassionate journey tailored to each patient, combining surgical excellence with a deep understanding of the personal challenges faced by those battling breast cancer.
Why We Love Dallas, TX
At Texas Breast Center, our affinity for Dallas, TX, is deeply rooted in the city’s unique character and dynamic growth. As the largest city in Dallas County and a key part of the Dallas–Fort Worth metroplex, Dallas stands out not only for its significant population and cultural diversity but also for its rich history and economic vibrancy.
Dallas, with a population exceeding 1.3 million, is a melting pot of cultures, ideas, and innovations. It’s the hub of a metropolitan area that is unparalleled in the Southern United States, both in terms of size and the absence of a navigable link to the sea. The city’s growth was initially spurred by the development of major railroad lines and later bolstered by the advent of the Interstate Highway System. These developments transformed Dallas into a crucial industrial, financial, and transportation center.
The city’s diverse economy is powered by sectors like defense, financial services, information technology, telecommunications, and transportation. Home to nine Fortune 500 companies, including prominent names like American Airlines Group, AT&T, and Texas Instruments, Dallas is a beacon of economic opportunity. Baylor Scott & White, our parent organization, is part of this thriving economic landscape. As the largest not-for-profit healthcare system in Texas, Baylor Scott & White’s presence in Dallas exemplifies the city’s role as a healthcare leader.
Education and diversity are at the heart of Dallas’ identity. The metropolitan area boasts over 41 colleges and universities, a testament to its commitment to education and innovation. The city is celebrated for its rich tapestry of racial, cultural, and religious backgrounds, hosting one of the largest LGBT communities in the U.S. In 2018, it was ranked as the fifth most diverse city in the nation by WalletHub.
Culturally, Dallas is a treasure trove. From the African American Museum to the Latino Cultural Center, and from the Dallas Museum of Fine Arts to the iconic State Fair of Texas held at Fair Park, the city’s cultural offerings are as diverse as its population. These cultural institutions not only enrich the lives of residents but also attract visitors from across the globe, adding to the city’s vibrant social fabric.
Being part of the Dallas-Fort Worth community is a source of pride for Texas Breast Center. The city’s dynamic blend of history, diversity, economic strength, and cultural richness makes it an ideal location for providing advanced and empathetic healthcare, just as we strive to do every day.
DRIVING DIRECTIONS FROM DOWNTOWN DALLAS
More FAQ’s About Dallas Breast Cancer Surgeon
What is the difference between a lumpectomy and a mastectomy, and how does Dr. Gorman decide which is best?
A lumpectomy involves removing the breast tumor and a small margin of surrounding tissue, while a mastectomy involves removing the entire breast. Dr. Gorman, a distinguished Doctor of Medicine, evaluates factors like the size and location of the tumor, the stage of malignancy, and the patient’s preferences. At Texas Breast Center, both procedures are performed with precision and care, aligned with the standards of the American Society of Breast Surgeons and the American College of Surgeons.
How does Texas Breast Center use imaging techniques like mammography, magnetic resonance imaging, and medical ultrasound in breast cancer diagnosis?
Imaging techniques are crucial in the medical diagnosis of breast cancer. Mammography is typically the first step, followed by more detailed imaging like magnetic resonance imaging (MRI) or medical ultrasound if a breast mass or abnormality is detected. At Texas Breast Center, Dr. Gorman utilizes these techniques to accurately identify and assess breast cancer, ensuring a comprehensive evaluation for each patient.
Can you explain the role of a biopsy in diagnosing breast cancer, and what types does Dr. Gorman perform?
A biopsy is essential for confirming a breast cancer diagnosis. Types include fine-needle aspiration, which uses a thin needle to extract tissue or fluid, and a core biopsy, where a larger needle is used. Dr. Gorman at Texas Breast Center also performs lymph node biopsies, including sentinel lymph node biopsies, to check for cancer spread. This aligns with her fellowship training in breast surgical oncology and her commitment to precise, minimally invasive diagnostic methods.
What is the importance of lymph node dissection and lymphadenectomy in breast cancer surgery?
Lymph node dissection and lymphadenectomy involve removing lymph nodes to check for cancer spread, which is vital for staging and treatment planning. Dr. Gorman, an expert in general surgery and breast cancer surgery, performs these procedures when necessary, with a focus on minimizing risk and maximizing outcomes. Her approach is informed by her residency at the University of Texas Southwestern Medical Center and her membership in the Society of Surgical Oncology.
What should I know about radiation therapy as a part of breast cancer treatment at Texas Breast Center?
Radiation therapy is often used after breast-conserving surgery like a lumpectomy to eliminate any remaining cancer cells. At Texas Breast Center, Dr. Gorman collaborates with radiation oncologists to tailor this treatment to each patient’s needs. She considers factors like the tumor’s location and the patient’s overall health to optimize outcomes, drawing on her extensive medical school training and experience in breast surgery.
How does Dr. Gorman address breast pain or nipple discharge in patients at Texas Breast Center?
Breast pain and nipple discharge can be symptoms of various breast conditions, not always cancer. Dr. Gorman evaluates these symptoms through a comprehensive assessment, including a physical examination and diagnostic imaging. Her approach reflects the best practices of the Association of Women Surgeons and preventive healthcare principles, ensuring that each patient receives accurate diagnosis and appropriate care.
Is preventive mastectomy an option at Texas Breast Center, and what are the considerations?
Preventive mastectomy is considered for individuals at high risk of developing breast cancer. Dr. Gorman assesses this risk based on factors like family history and genetic predisposition. As a surgeon affiliated with a top-tier hospital in North Texas, she ensures that her patients are fully informed about this option, supporting them through the decision-making process with empathy and expertise.
How do cancer centers like Texas Breast Center approach the treatment of breast cancer, and what role do breast specialists play?
Cancer centers, including Texas Breast Center, approach the treatment of breast cancer with a comprehensive strategy. Breast specialists like Dr. Gorman collaborate with a team of experts in medical oncology, radiation therapy, and reconstructive or plastic surgery to offer personalized treatment plans. This team approach ensures each aspect of breast cancer, from diagnosis to surgical management, is handled with utmost care and expertise.
Can you explain the importance of breast cancer staging and how it guides treatment decisions at Texas Breast Center?
Breast cancer staging is crucial in determining the extent of the cancer and the most effective treatment strategy. At Texas Breast Center, staging is conducted through advanced breast imaging techniques, including breast MRI, and breast biopsy. Dr. Gorman, along with her team, uses this information to plan targeted therapy, surgery, and other treatments, ensuring each patient receives the most appropriate care for their specific stage of cancer.
What options are available for reconstructive surgery and oncoplastic surgery at Texas Breast Center?
Reconstructive surgery and oncoplastic surgery are vital components of breast cancer treatment for many patients. At Texas Breast Center, Dr. Gorman offers a range of options for breast reconstruction, combining oncology research insights and surgical expertise to achieve the best aesthetic and functional outcomes. Her approach to oncoplastic surgery focuses on removing cancer while preserving or restoring the breast’s appearance.
How does genetic testing and genetic risk evaluation factor into breast cancer treatment at Texas Breast Center?
Genetic testing and risk evaluation are integral in assessing a patient’s susceptibility to breast cancer. Texas Breast Center, under Dr. Gorman’s guidance, utilizes genetic testing to identify patients with a higher genetic risk for breast cancer. This information is crucial in tailoring preventive strategies and treatment plans, including decisions about preventive mastectomy and targeted therapy.
In terms of education and training, how does Dr. Gorman’s background and residency programs contribute to her expertise as a breast cancer surgeon?
Dr. Gorman’s educational background, including her residency programs and training at prestigious institutions like UT Southwestern Medical Center, has equipped her with deep knowledge and skills in the surgical management of breast cancer. Her extensive training in general surgery and breast surgery, combined with ongoing participation in breast cancer research and oncology research, ensures that she remains at the forefront of advancements in breast cancer care.
What is the approach to benign breast conditions and cancer awareness at Texas Breast Center?
At Texas Breast Center, benign breast conditions are treated with the same level of care and attention as cancerous conditions. Dr. Gorman and her team provide thorough evaluations and treatment options for breast lumps and other non-cancerous breast issues. Additionally, the center actively participates in cancer awareness initiatives, educating the community about breast health, early detection, and the importance of regular breast imaging and breast exams.


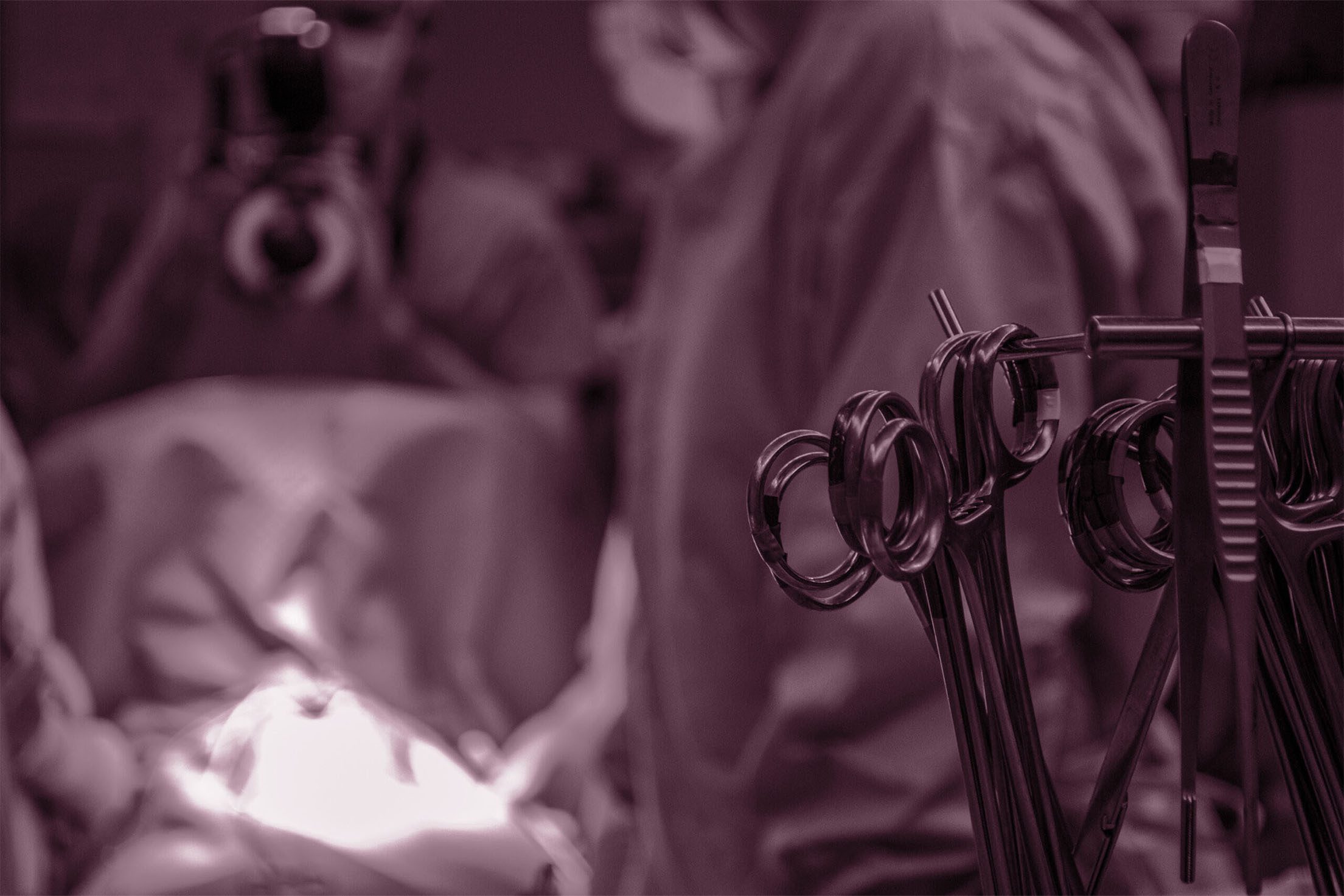
 The public conception of breast cancer treatment is quite positive; people are confident that medical science has achieved a reasonable degree of success at dealing with breast cancer, and so ironically many women express more concern about how their body will look postoperative.
The public conception of breast cancer treatment is quite positive; people are confident that medical science has achieved a reasonable degree of success at dealing with breast cancer, and so ironically many women express more concern about how their body will look postoperative.
 Surgery of any kind always involves some degree of risk, and Breast Cancer surgery is no different in that regard. The good news is that the vast majority of breast cancer surgeries across the world are completed successfully without any complications. Generally speaking, when any complications do arise, they tend to be minor and easy to deal with from a medical standpoint.
Surgery of any kind always involves some degree of risk, and Breast Cancer surgery is no different in that regard. The good news is that the vast majority of breast cancer surgeries across the world are completed successfully without any complications. Generally speaking, when any complications do arise, they tend to be minor and easy to deal with from a medical standpoint.
 Humans by their very nature do not like the unknown, which might explain why one of the most frequent questions we are asked at the Texas Breast Center is what to expect regarding your lumpectomy surgery recovery.
Humans by their very nature do not like the unknown, which might explain why one of the most frequent questions we are asked at the Texas Breast Center is what to expect regarding your lumpectomy surgery recovery.